The Devastating Effects of Benzodiazepine Abuse
- Written by: Alexandra Talarico
- Medically Reviewed by: Ashley Gardner
- Compliance Reviewed by: Marianne Birmingham
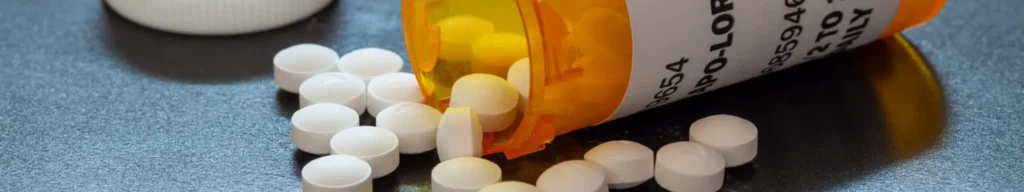
Benzodiazepines were involved in 8,613 overdose deaths in the United States in 2019
Benzodiazepines are a type of prescription medication used to treat anxiety, insomnia, and other related conditions. While they are effective when used as prescribed, their misuse can cause severe physical and psychological harm.

Contact Recovery Centers of America Today
If you are struggling with benzodiazepines, it is essential to seek medical help and support immediately. Recovery Centers of America’s team of medical and mental health professionals is here to provide comprehensive addiction care to help you overcome substance use disorder and achieve long-term recovery.
- Contact 1-800-RECOVERY to speak with a treatment advisor 24/7/365
- No cost intervention services available exclusively through RCA
- Verify your insurance benefits here
- One of our transportation specialists will pick you up wherever you are in 2 hours or less
Don’t wait another day to get the help you need. Contact the RCA team today to begin the journey towards a healthy, fulfilling life. We are committed to supporting you every step of the way, providing personalized treatment options and evidence-based therapies to help you achieve your goals.
Together, we can overcome your benzodiazepine addiction and build a brighter future.
Contact Recovery Centers of America now and take the first step towards long-lasting recovery.
An Evidence-Based Continuum
Our Unique System of Care, Guided by The RCA Care Model
The Core Tenets of Our Care Model
There are six core tenets that we’ve determined to be essential for every patient to achieve sustained recovery.
Medications for Addiction Treatment
Medication to help reduce cravings, maintain long-term recovery, and decrease the likelihood of relapse.
12-Step Recovery Support
The 12 steps and other recovery support programs are integrated throughout the process, with meetings held daily.
Dialectical Behavior Therapy (DBT) Skills
Evidence-based skills training and coaching to help manage emotions, cope with crisis, and improve relationships.
Family Involvement
Family support services including engagement, education, support groups, and other resources.
Alumni
The Alumni program helps ease the transition back into daily life and provides long-term sober supports.
Measurement-Driven Care
Industry leading measurement methods track patients’ success and incorporate data into treatment feedback.
Our caring and experienced staff are dedicated to providing personalized care to each person struggling with addiction to promote a healthy and sustainable recovery.
Don’t let drugs or alcohol control your life – contact Recovery Centers of America today to get the help you or your loved one needs to start on the path to recovery.

How Benzodiazepines Negatively Impacts Your Life

Physical

Psychological

Financial
Social
The Truth About Benzodiazepines
In 2021, nearly 14% of overdose deaths involving opioids also involved benzodiazepines, a type of prescription sedative commonly prescribed for anxiety or to help with insomnia.
Benzodiazepines were involved in 8,613 overdose deaths in the United States in 2019
Long-term use of benzodiazepines is associated with an increased risk of death from respiratory disease and cancer
An estimated 5.4 million people ages 18 or older misused benzodiazepines at least once in 2019
Benzodiazepine addiction
Unfortunately, it is incredibly easy to become addiction to benzodiazepines, commonly called benzos.
According to research, when you takes a benzo, their dopamine levels surge, resulting in a flood of those feel-good neurotransmitters hitting your brain. Researchers also believe that as benzos accumulate in the body, they can actually change the structure and function of certain receptors in the brain. The changes make these receptors even more prone to excitable surges from other neurotransmitters. In other words, future dopamine rushes are intensified and increased.
All of this adds up to one thing: An intense high that many people do not want to part with. What’s even scarier is how quickly tolerance can happen. In just about 6 months of benzo use, tolerance can develop – though it is very possible for physical dependence to happen sooner. In fact, an estimated 44% of users become dependent on benzos.
Because benzos are a part of the prescription sedative class of drugs, they have a calming effective. While benzo addiction symptoms range from physical, psychological, and behavioral symptoms, they might include:
- Anxiety
- Depression
- Insomnia
- Increased heart rate and blood pressure
- Excessive sweating
- Hand tremors
- Hallucinations
- Seizures
Benzodiazepine abuse
More and more people are being prescribed benzos on a daily basis – and staying on them for years. Now, doctors are beginning to see a new trend associated with benzo use: cognitive impairment. Patients are forgetting things they were once able to easily recall and forgetting how to perform tasks they are familiar with. When researchers dug deeper into this, they found consistent links between doses of benzos and cognitive deficiencies. Here’s the scariest part: Study participants who were both older and younger than 60 had the same impairment because of the benzo use.
But that isn’t all. There was a sharp increase in long-term use benzo prescriptions in the elderly- 14.7% of people ages 18-35 vs 31.4% of people ages 65-80. A study of this found that the more a person took benzo, the higher the risk was for developing Alzheimer’s – 84% higher to be exact.
If the risk of addiction, tough withdrawal symptoms, cognitive impairment and damage, and a severe risk of Alzheimer’s wasn’t enough, there is also the risk of early death. A study examined over 100,000 participants medical records and found that benzos were associated with the greatest number of early deaths among all the prescription medications tested. In fact, the study showed that the chances of an early death double with a prescription of benzodiazepines.
Need Addiction Treatment? We are here 24/7
Benzodiazepine withdrawal
Like with most drugs, trying to get off benzos can be extremely difficult. Once your body has become dependent on the drug, detoxification needs to be handled carefully and medically. Benzo withdrawal symptoms can include:
- Sweating
- Nausea
- Headache
- Muscular pain
- Stiffness
- Difficulty concentrating
- Perceptual changes
- Sleep disturbance
- Irritability
- Increased tension and anxiety
- Panic attacks
- Heart palpitations
- Muscle tremor
Depending on the dose of medication, benzo withdrawal could be worse, leading to seizures and psychosis. Other factors that’ll impact how severe withdrawal are how long you’ve been taking the medication, if you’re on more than one benzo or other types of sedating drugs, any other substance abuse issues, and if you are quitting more than one substance at a time.
Benzo withdrawal timeline
Even if you’re on a small dose of benzos prescribed by your doctor, you can still experience dangerous withdrawal symptoms after only a month of use. A benzo withdrawal timeline depends on the type of benzo you’re taking. For example, if you’re taking a shorter-acting benzo like alprazolam (more commonly known as Xanax) or lorazepam (also called Ativan), these tend to leave the system quicker. That’s bad news for benzo withdrawal symptoms, because that means symptoms can pop up in as little as 8 hours.
If you’re taking a longer-acting benzo such as clonazepam (Klonopin), these tend to stay in the body longer. That means it might be a day or two before withdrawal symptoms begin to show. The American Psychiatric Association found that some people experience withdrawal symptoms for several weeks.
Benzos and alcohol
According to a SAMHSA study, there has been a steady increase in the misuse of benzos and alcohol. The data from SAMHSA found there are a few different reasons why people combine alcohol and benzos, including:
- To enhance the effects of at least one, if not both, of the drugs.
- The misconception that mixing prescription drugs, like benzos, with other drugs is safer than mixing illicit drugs with alcohol or other drugs.
- Enhanced psychoactive effects when mixing benzos and alcohol.
The dangers of mixing benzos and alcohol should not be taking lightly. You’ve likely noticed that every single warning label on benzo containers cautions against mixing the benzo with alcohol. In fact, odds are, when a physician prescribes it, they will likely strongly advise against mixing with alcohol. Here are a few reasons why mixing benzos and alcohol can be deadly:
Heightened effects:
Mixing any two drugs will enhance the effects of each one. Since alcohol and benzos have the same mechanism of action results, mixing the two will heightened the effects of each one.
Bigger risk of overdose:
Mixing two central nervous system depressants – such as benzos and alcohol – puts the user at extreme risk for overdose. Also, the amount of alcohol that can cause an overdose is less when taken with benzos – same with the amount of benzos that can cause an overdose when taken with alcohol.
Side effects can increase:
When you mix two central nervous system depressants, the possible side effects are going to be enhanced. These side effects could be vomiting, nausea, lethargy, allergic reactions, and more. Unpredictable side effects are possible, too.
Significant reduction in cognitive abilities:
With the heightened effects of both drugs, the user will experience a massive decrease in their cognitive abilities. This could mean accidents happening, risky decisions or poor behaviors, decrease in reasoning abilities, or inability to control emotions, resulting in aggression or hostility. Motor coordination is affected, too.
There are several other complications when mixing benzos and alcohol, including heart attack, stroke, suicidal tendencies, seizures, live damage, kidney damage, depression, bipolar disorder, anxiety disorders, and more.
Is Xanax a benzo?
Yes, Xanax is a benzo and is generally prescribed to treat anxiety disorders, panic attacks, and insomnia. A person’s body will quickly develop a tolerance to Xanax, meaning more medication will be required in order to get the same effect. Both a physical and an emotional dependence are developed when taking this drug.
Is Ambien a benzo?
No, Ambien is a non-benzo drug that was created to have the same effectiveness as other benzos, like Xanax, but without the same hazardous and habit-forming properties. However, Ambien is still considered an addictive substance – it just takes a bit longer to develop an addiction to Ambien than to benzos.
Is Ativan a benzo?
Yes, Ativan is a benzo and is the brand name for the prescription drug lorazepam. Ativan interacts with chemicals within the brain to treat anxiety disorders or other anxiety that is associated with depression. Unfortunately, Ativan is very addictive, but because it’s legal, a lot of people don’t realize they’re abusing it or even addicted to it.
Is Clonidine a benzo?
Clonidine is an antihypertensive that’s often used as an alternative to benzos. However, just because it isn’t as habit-forming as others doesn’t mean it can’t be abused. It’s used to treat ADHD, dysmenorrhea, Tourette’s syndrome, menopausal hot flashes, high blood pressure, and certain anxiety disorders.
Is Lorazepam a benzo?
Yes. Lorazepam is the generic name for Ativan and is an anti-anxiety medication within the benzo family.
Do all benzodiazepines show up the same on a drug test?
It depends on the type of test. For example, blood tests have the shortest window of drug detection, while hair tests have the longest. Urine (or urinalysis) have an intermediate testing window. However, the everyday standard urine test doesn’t pick up on every benzo. According to the URMC, many common tests may not find Xanax, Klonopin, Restoril, or Halcion.
How long do benzos stay in urine?
First, it’s important to answer this question first: How long do benzos stay in your system? The short answer is, benzos can stay in your system for up to 10 days; however, hair tests can actually show evidence of benzos for up to 90 days. Benzos will appear in blood samples for 24 hours and saliva for 2.5 days.
As for how long benzos stay in urine, benzos can sometimes produce a positive urine test result in as little as 2-7 hours after someone has taken the drug. However, the length of time for detection depends on a few things. For example, if you take a longer-acting benzo such as Valium, this will stay in your urine for up to 10 days. On the other hand, shorter-acting benzos like Halcion are generally only detected for 48 hours.
Once your body metabolizes the drug, approximately one-fifth of the oral dose taken stays in the urine. If you’re on a lower dose of Xanax, you might test positive for it up to 4 days after you’ve taken it. However, if you take a heavy dose, you may test positive for Xanax a week after use.
It’s important to keep in mind that metabolism plays a huge role in how long benzos stay in your urine. Everyone’s metabolism is different and depends on a variety of characteristics, including gender, age, ethnicity, and more. If you have a slower metabolism rate, that could mean benzos (and other drugs) will stay in your urine for longer.





